6 Sept 2021
Pancreatitis in dogs

Pancreatitis is common in canine medicine1,2. Its overall prevalence has been estimated as 0.8% in dogs, being higher in some specific breeds such as miniature schnauzers, Yorkshire terriers or cocker spaniels2.
However, diagnosis of pancreatitis can be very challenging – especially if we want to conclude pancreatitis as a cause of the clinical signs. Diagnosis becomes even more difficult for chronic cases. Subclinical cases are also detected in postmortem and the consequences of failing to diagnose it are unknown. Equally, perhaps inflammation of the pancreas is present (the definition of pancreatitis), but that is not the cause of the problems.
As sometimes said, it is not about finding “an answer”, it is about finding “the answer”. This article will be focused mainly on acute cases.
Clinical signs for pancreatitis vary widely, as does its severity. Common signs of acute pancreatitis are vomiting, abdominal pain and lethargy.
Considering blood tests, lipase and amylase are not pancreas-specific, and considerable variability exists regarding their respective sensitivity and specificity in the veterinary literature; a high background of enzyme activity from non-pancreatic sources exists.
Renal disease and prerenal azotaemia can cause increased levels of lipase and amylase as both enzymes are excreted via the kidney. Only elevation exceeding three to five times the normal range is considered suggestive of pancreatitis in dogs3.
Nowadays, canine pancreatic lipase immunoreactivity (cPLI) is considered a better marker of pancreatitis, but a high trypsin-like immunoreactivity is highly suggestive of pancreatitis in dogs3. Spec cPL/SNAP cPL are organ-specific and only measure the lipase of pancreatic origin.
Accumulating evidence exists that cPLI is the most sensitive and specific test for canine pancreatitis, although its sensitivity varies depending on the severity and chronicity of the disease3. A recent new type of lipase assay (1,2-o-dilauryl-rac-glycero-3-glutaric acid-(6’-methylresorufin) ester [DGGR] lipase) showed a good agreement with Spec cPL.
Ultrasound is the most useful imaging tool in diagnosis of pancreatitis and it helps ruling out/in other differential diagnoses or to diagnose comorbidities. Some findings suggestive of acute pancreatitis are pancreatic enlargement, hypoechogenicity, irregularity, and hyperechoic fat and mesentery surrounding the pancreas.
In summary, diagnosis of pancreatitis as a unique cause of a clinical complaint is based on exclusion of other differential diagnoses and combining different diagnostic tools – usually bloods and imaging (such as DGGR lipase and abdominal ultrasound).
Treatment
Treatment of this condition is sometimes as challenging as the diagnosis. When discussing treatment of pancreatitis with the owner, it is important to emphasise some points:
- The severity of this disease is extremely variable, but it is usually possible to estimate the severity at admission. It is then possible to have a subjective discussion of the prognosis and length of hospitalisation. A clinical severity index was shown to correlate with days of hospitalisation4.
- The cornerstone of management is supportive treatment to alleviate the signs and control complications. No specific treatment or medication exists for pancreatitis.
- Time. Some cases may improve quicker than others. Sometimes, patients need very long periods of hospitalisation – even reaching two weeks in some cases.
Supportive treatment includes the following.
Nutrition to counterbalance catabolic effects of the disease
If the dog is clinically stable, a short anaesthesia to place an oesophagostomy tube (and epidural catheter +/− central line) would be the option of choice. Dogs fed via oesophagostomy tube improved faster than dogs receiving parenteral nutrition1. In cases where anaesthesia is not considered safe, a nasoesophageal/gastric tube can be placed (Figure 1).

In humans and dogs with critical illness, lack of enteral nutrition has been shown to perpetuate systemic inflammation, as well as lead to mucosal atrophy and other changes5. If vomiting is very severe, a jejunostomy tube or parenteral nutrition should be considered. Due to the invasiveness of the former option, parenteral nutrition is usually elected. Not many studies on dietary preference exist, but a balanced, extra low-fat diet would be the diet of choice.
Analgesia
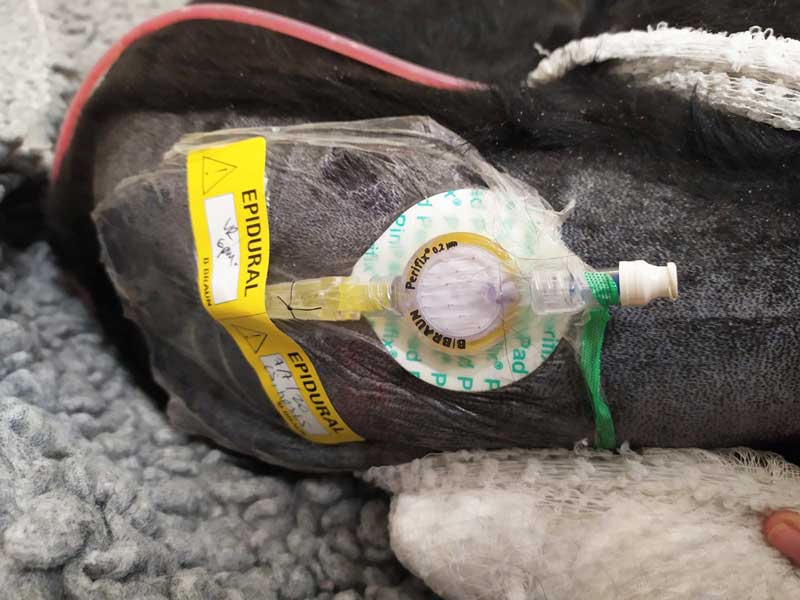
Buprenorphine or methadone can be used in mild cases of pancreatitis. If the patient has a lot of pain, a constant rate infusion of ketamine or lidocaine – and, if equipment and skill allow, epidural catheter – should be considered (Figure 2).
It is important to prescribe analgesia, even if the patient does not appear to have pain, as it is sometimes difficult to detect it. Pain scoring systems can also be used to ensure the analgesia prescribed is adequate.
Fluid therapy as deemed appropriate
The percentage of dehydration should be estimated, along with ongoing losses, and added to the maintenance volume. Supplementation with potassium may be needed based on biochemistry results.
In a human study, alkalinising fluids (for example, Hartmann’s) showed a better response compared to acidifying solutions (for example, sodium chloride 0.9%) so the same conclusion may be drawn in dogs5. Severe cases may develop pleural effusion or acute kidney injury, so urinary catheter placement may need to be considered for a better management of the ins and outs.
Antiemetic therapy
Regarding antiemetic therapy, maropitant would be the first option due to its mechanism of action and the role of substance P in mediating vomiting. Ondansetron could be used in refractory cases.
Metoclopramide would be another option, but it could be argued that in humans it affects the sphincter of Oddi and be contraindicated in cases of pancreatitis. Metoclopramide can be useful if concomitant gastrointestinal ileus exists because of its prokinetic effect.
Antibiotics or fresh frozen plasma
Use of antibiotics or fresh frozen plasma (FFP) were commonly considered in the past; however, no evidence of a benefit to using these treatments exists. Antibiotics should only be used if evidence of infection and FFP is present for cases where concurrent coagulation abnormalities exist. No evidence exists to support the use of omeprazole unless melena or haematemesis is present.
In 2019, a study with 65 dogs showed a decreased one-month mortality, earlier improvement of clinical signs and earlier reduction of C-reactive protein in dogs treated with prednisolone (1mg/kg once a day)6. However, this study was a non-blinded, non-randomised study and further studies are needed to confirm the findings; however, it is a treatment strategy to be kept in mind.
Possible complications of pancreatitis include aspiration pneumonia due to aspiration of vomit, pleural effusion or acute kidney injury (the final two due to development of systemic inflammatory response syndrome).
Some scenarios exist where surgical management may be discussed:
- In cases of pancreatic abscess, surgery should be recommended, but the prognosis is considered poorer, with a mortality between 50% and 86%2. However, they are uncommon.
- In cases of quite severe extrahepatic biliary obstruction not responding to medical treatment, stent placement to open the peripancreatic bile duct can be considered.
However, surgery should be considered as a last option of management in cases of pancreatitis.
Conclusion
Pancreatitis is a common disease for which the treatment is based around supportive care and detection/control of possible complications.
Disease severity varies considerably, but it can be a life-threatening condition. The challenges of its clinical diagnosis makes the development of more standardised studies about treatment difficult.
- Some drugs are used under the cascade.
